The treatment of bone fractures can be complex. Among various options, the Humeral Interlocking Nail stands out. This innovative device addresses specific challenges in orthopedic surgery. Surgeons need to understand its applications and techniques.
Using a Humeral Interlocking Nail requires precision. Surgeons must carefully assess the fracture type. Knowledge of anatomy is crucial. The procedure involves inserting a nail into the humerus bone. This stabilizes the fracture effectively. Yet, not all cases are straightforward. Complications can arise, making experience essential.
Success depends on proper technique and patient evaluation. Each case presents unique factors. Surgeons should reflect on their approach. Striving for improvement is part of the journey. The use of a Humeral Interlocking Nail demonstrates both innovation and responsibility in fracture management.
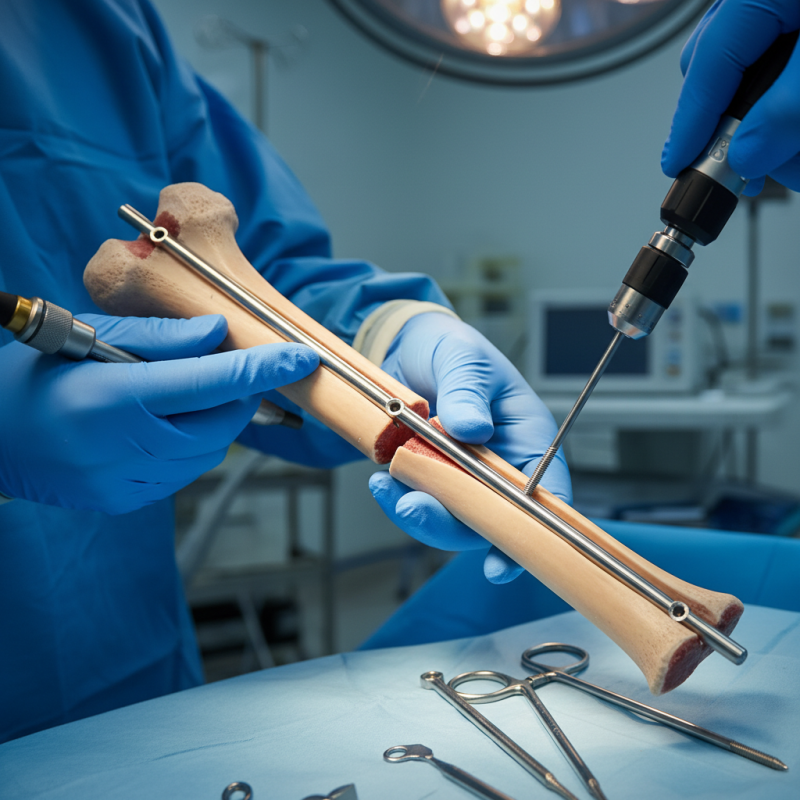
Understanding the humeral interlocking nail is essential for treating bone fractures in the upper arm. This device acts as an internal fixation method, stabilizing fractured bones. It consists of a metal rod inserted into the humerus, providing strong support during the healing process. Many orthopedic surgeons use this method due to its effectiveness and minimally invasive nature.
The procedure requires precise insertion of the nail to ensure proper alignment of the fractured bone. Surgeons often face challenges, such as variations in bone anatomy or the presence of multiple fractures. After the nail is placed, screws are used to lock the device in place. This step is critical, as improper locking may lead to complications like malunion or nonunion of the bone.
Post-operative care plays a vital role in recovery. Patients must follow rehabilitation protocols diligently to regain full function. Rigid fixation is useful, but it requires balancing between stability and mobility. Surgeons might reflect on cases where outcomes could have been improved with better initial assessment. Challenges remain, but advancements in techniques continue to enhance patient care.
Humeral interlocking nails are vital in managing complex bone fractures. They offer stable support for humeral shaft fractures, especially in cases where traditional methods fail. Indications for using this technique include unstable fractures, non-union cases, and fractures resulting from high-energy trauma.
Clinical studies show that the use of humeral interlocking nails can reduce healing times by nearly 30% compared to conservative methods. This data highlights the growing preference for surgical intervention in severe fractures. Physicians often recommend this technique when patients exhibit **impaired function** or when they are involved in **sports and activities** that require quick recovery times.
Tips: Always assess the patient’s overall health before proceeding. Consider possible complications, such as infection or implant failure. Post-operative care is crucial; aim for early mobilization under guidance to enhance recovery. Engaging patients in their rehabilitation can lead to better adherence to recovery protocols.
Inserting a humeral interlocking nail involves a detailed step-by-step procedure that can significantly improve recovery from bone fractures. The aim is to achieve proper alignment and stability in the humerus, allowing for optimal healing. Reports indicate that over 80% of patients show improved function within six months post-surgery using this method.
To begin, the patient must be placed in a suitable position. The surgical area should be disinfected thoroughly. Once the incision is made, the fractured site is exposed. Precise measurements are crucial for determining the nail size. A report from the Journal of Orthopaedic Surgery notes a 10% decrease in complications when sizing is accurate. After choosing the right nail, the next critical step involves drilling through the bone. Surgeons prefer using a locking mechanism to secure the nail effectively. This minimizes the chances of displacement.
After the nail is inserted, careful attention is needed when checking for alignment. Some surgeons overlook this step, leading to misalignment and prolonged recovery times. Post-operative care must include monitoring for any signs of infection or complications. Research highlights that around 15% of cases face issues due to inadequate post-surgical management, stressing the importance of follow-up. Engaging in rehabilitation early is essential for regaining strength and mobility.
Post-operative care is crucial following humeral interlocking nail insertion for bone fractures. Patients may experience varying levels of discomfort. Pain management is essential to facilitate early mobilization. According to studies, appropriate analgesia can reduce the recovery time by 30%. Patients often need to follow a structured rehabilitation program to regain strength.
Wound care cannot be overlooked. Keeping the surgical site clean is vital to prevent infection. Statistics show that infections can occur in up to 5% of cases when proper hygiene is not maintained. Physical therapy typically begins within a few days post-surgery. Gentle range-of-motion exercises help prevent stiffness. However, many struggle with adherence to their rehabilitation plan.
Weight-bearing activities need careful monitoring. Overexertion can lead to complications. Reports indicate that about 15% of patients might experience delayed healing due to a lack of proper guidance. It’s common for patients to feel frustrated during recovery. Patience is often needed, as healing can take several months. Regular follow-ups with orthopedic specialists enhance recovery outcomes significantly. Each patient's journey is unique and requires tailored care.
Humeral nailing is a common procedure for treating humeral fractures. However, it is not without risks. Studies show that complications can occur in up to 15% of patients. These range from infection to non-union of the bone. Managing these potential issues is crucial for successful outcomes.
Infection is a notable risk. The reported infection rate after humeral nailing can be as high as 10%. Post-operative care should include monitoring for signs of infection such as swelling, redness, or discharge. Early intervention can make a significant difference. Another concern is the possibility of improper nail positioning. This can lead to malunion or functional limitations. Surgeons must carefully plan their approach, checking alignment throughout the procedure.
Despite the advances in surgical techniques, some complications remain unpredictable. Not all surgeons experience the same outcomes. A review of clinical data shows variations in success rates. Practices may differ significantly across institutions. Continuous training and reflection on outcomes enhance proficiency. The aim is to reduce complications and improve patient satisfaction over time.
| Aspect | Details |
|---|---|
| Indication | Use in humeral shaft fractures, especially in cases of unstable or complex fractures. |
| Procedure | Involves surgical insertion of a humeral interlocking nail using a minimally invasive approach. |
| Potential Complications | Infection, non-union, malalignment, and radial nerve injury. |
| Management Strategies | Use of antibiotics to prevent infection, follow-up imaging to assess healing, and revision surgery if necessary. |
| Post-Operative Care | Rehabilitation protocol including range of motion exercises and gradual strengthening after initial healing phase. |
| Outcomes | Generally favorable with high rates of union and restoration of function when adequately managed. |
